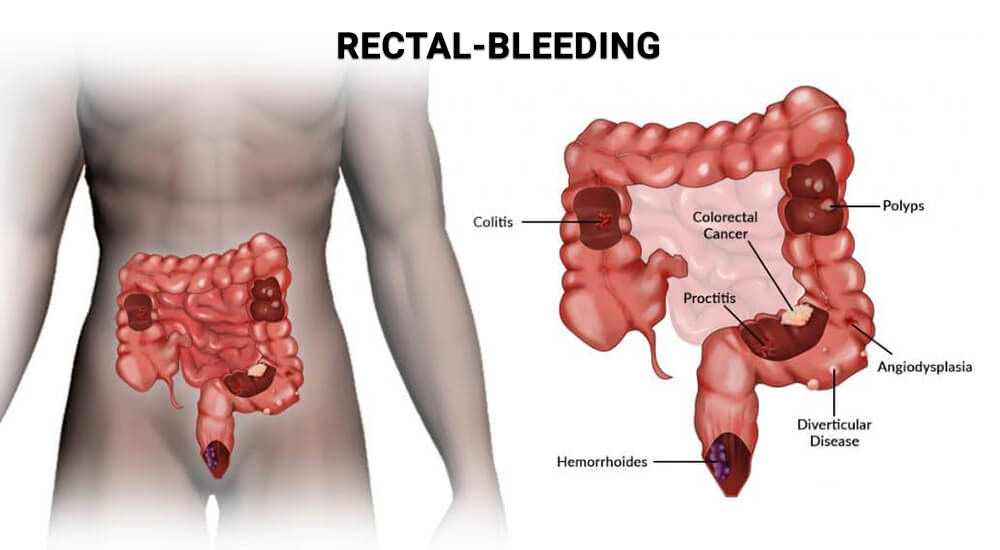
What is Rectal Bleeding?
Rectal bleeding, sometimes called colorectal bleeding, means blood is passing from the anus or lower digestive tract. Patients may notice bright red blood on toilet paper, blood in the toilet bowl, blood coating the stool, blood mixed with stool, or dark/black stools.
Rectal bleeding is a symptom, not a diagnosis. Hemorrhoids and anal fissures are common causes, but bleeding can also come from colon polyps, inflammatory bowel disease, diverticular disease, infection, or colorectal cancer.
Dr. Aisha Akhtar, a colorectal surgeon in Phoenix, evaluates rectal bleeding, blood in stool, hemorrhoid bleeding, and other anorectal symptoms for patients in Phoenix, Scottsdale, Glendale, and surrounding Arizona communities. Because the cause is not always obvious, persistent or unexplained bleeding should be evaluated.
Why Am I Seeing Blood When I Wipe?
Seeing bright red blood on toilet paper is one of the most common ways rectal bleeding appears. This can happen with hemorrhoids, anal fissures, irritation from wiping, constipation, or straining.
Blood when wiping may be more likely from an anal or rectal source when it is:
- Bright red
- Seen on toilet paper
- Seen after a bowel movement
- Associated with anal pain, itching, or a lump
- Triggered by constipation or hard stool
Even when bleeding looks minor, it should not automatically be assumed to be hemorrhoids, especially if it is recurrent, persistent, mixed into stool, or associated with other symptoms.
How Rectal Bleeding May Appear
The appearance of bleeding can provide clues about the possible source, although it does not confirm the diagnosis.
| What You Notice | Possible Source |
|---|---|
| Bright red blood on toilet paper | Hemorrhoids, fissure, anal irritation |
| Bright red blood in toilet bowl | Hemorrhoids, fissure, rectal source |
| Blood coating the stool | Rectal or lower colon source |
| Blood mixed within stool | Possible colon source |
| Dark red or maroon stool | Bleeding higher in the colon |
| Black, tarry stool | Possible upper gastrointestinal bleeding |
These patterns help guide evaluation, but an exam or colonoscopy may be needed depending on age, risk factors, and symptoms.
Common Causes of Rectal or Colorectal Bleeding
Rectal bleeding can come from the anus, rectum, colon, or sometimes higher in the digestive tract.
Hemorrhoids
Hemorrhoids are one of the most common causes of bright red rectal bleeding. Bleeding from internal hemorrhoids is often painless and may appear on toilet paper, on the stool, or in the toilet bowl.
Learn more:
Anal Fissures
An anal fissure is a small tear in the anal lining. Fissures often cause sharp pain during bowel movements, burning afterward, and bright red blood with wiping.
Colon Polyps
Colon polyps are growths in the colon or rectum. Some polyps can bleed, and certain types can develop into colorectal cancer over time. Polyps are usually diagnosed and removed during colonoscopy.
Colorectal Cancer
Colorectal cancer can sometimes cause rectal bleeding, blood mixed with stool, changes in bowel habits, anemia, weight loss, or abdominal symptoms. Bleeding should be evaluated carefully, especially in adults age 45 or older or those with a family history.
Diverticular Disease
Diverticular bleeding can cause sudden rectal bleeding, sometimes in larger amounts. It is more often painless but may require urgent evaluation if bleeding is heavy.
Inflammatory or Infectious Colitis
Inflammation of the colon or rectum can cause bleeding, mucus, urgency, diarrhea, abdominal pain, or cramping. Causes may include ulcerative colitis, Crohn’s disease, infection, ischemic colitis, or proctitis.
Learn more:
Is It Hemorrhoids or Something More Serious?
Hemorrhoids are common, but not all rectal bleeding is hemorrhoidal.
Bleeding may need more complete evaluation if you have:
- Blood mixed within stool
- Dark red or black stool
- Persistent or recurrent bleeding
- New change in bowel habits
- Unexplained weight loss
- Fatigue or anemia
- Abdominal pain
- Family history of colorectal cancer or advanced polyps
- Age 45 or older and not up to date on colorectal cancer screening
A colorectal specialist can evaluate the anorectal area and determine whether anoscopy, colonoscopy, or another test is appropriate.
Learn more:
When to Seek Medical Care for Rectal Bleeding
Schedule evaluation if you have:
- Recurrent or persistent rectal bleeding
- Bright red blood that keeps coming back
- Blood mixed within stool
- Dark red, maroon, or black stool
- Rectal bleeding with abdominal pain
- Rectal bleeding with weight loss, fatigue, or anemia
- Bleeding with a change in bowel habits
- Rectal bleeding after age 45
- Family history of colorectal cancer or advanced polyps
Seek urgent care or emergency evaluation if bleeding is heavy, you feel faint or weak, or you have severe abdominal pain, fever, or signs of significant blood loss.
Learn more:
How Rectal Bleeding Is Evaluated
Evaluation begins with a careful history and physical examination. The goal is to identify whether the bleeding is coming from hemorrhoids, fissure, rectal inflammation, colon disease, or another source.
Depending on symptoms, evaluation may include:
- Review of bleeding pattern and bowel habits
- Medication review, including blood thinners
- Family history and cancer screening history
- External anal examination
- Digital rectal examination
- Anoscopy to look for hemorrhoids, fissures, or rectal inflammation
- Flexible sigmoidoscopy in selected cases
- Colonoscopy when full colon evaluation is needed
Colonoscopy may be recommended if bleeding is persistent, unexplained, mixed with stool, associated with warning symptoms, or if the patient is due for colorectal cancer screening.
Learn more:
What to Expect During Your Visit
During a visit for rectal bleeding, Dr. Akhtar will review when the bleeding started, how it appears, whether it is painful, and whether it is associated with constipation, diarrhea, abdominal pain, weight loss, or a change in bowel habits.
The visit may include:
- Focused symptom review
- Review of prior colonoscopy or screening history
- External anorectal exam
- Digital rectal exam when appropriate
- In-office anoscopy if needed
- Discussion of whether colonoscopy is recommended
Many anorectal causes of bleeding can be identified during an office visit. If the bleeding pattern suggests a colon source, further evaluation may be recommended.
Treatment Options for Rectal Bleeding
Treatment depends on the cause of bleeding.
Common treatment approaches include:
- Hemorrhoids: Fiber, hydration, stool regulation, topical therapy, rubber band ligation, or surgery when needed
- Anal fissures: Stool softening, topical medication, sitz baths, and treatment to relax the anal sphincter when appropriate
- Colon polyps: Removal during colonoscopy
- Inflammatory bowel disease: Medical therapy and long-term monitoring
- Infectious or inflammatory colitis: Treatment based on the specific cause
- Diverticular bleeding: Observation, colonoscopy, or hospital-based treatment depending on severity
- Colorectal cancer: Surgery, chemotherapy, radiation, or combined treatment depending on stage and location
The most important step is identifying the cause before starting treatment.
What Happens After Treatment?
Outcomes depend on the cause of rectal or colorectal bleeding.
- Hemorrhoids and anal fissures: Most patients improve with fiber, stool regulation, topical therapy, or minor office procedures. Recurrence is less likely when constipation, straining, diarrhea, or prolonged toilet sitting are addressed.
- Colon polyps: Removal during colonoscopy is usually effective and may reduce future colorectal cancer risk, although surveillance colonoscopy may be needed based on the number, size, and type of polyps.
- Inflammatory bowel disease: Symptoms can often be controlled with medical therapy, but long-term monitoring is important because bleeding may recur during flares.
- Colorectal cancer: Prognosis depends strongly on the stage at diagnosis. Earlier detection is associated with better treatment options and improved survival.
Appropriate evaluation is important because treatment and prognosis differ significantly depending on the source of bleeding.
Can Rectal Bleeding Go Away on Its Own?
Sometimes bleeding from hemorrhoids or a small fissure improves when constipation, diarrhea, or straining improves. However, bleeding that stops temporarily can still come back if the underlying cause is untreated.
You should not rely only on symptom improvement if bleeding is recurrent, unexplained, or associated with warning signs. A clear diagnosis helps avoid missing a more serious condition.
Rectal Bleeding Evaluation in Phoenix, Scottsdale & Glendale
Dr. Aisha Akhtar evaluates rectal bleeding, colorectal bleeding, blood in stool, hemorrhoid bleeding, fissures, and other anorectal symptoms for patients in:
- Phoenix, AZ
- Scottsdale, AZ
- Glendale, AZ
- Surrounding Arizona communities
If you are seeing blood when wiping, blood in the toilet, or blood mixed with stool, a colorectal evaluation can help identify the cause and guide treatment.
Frequently Asked Questions
Is bright red blood usually hemorrhoids?
Bright red blood is often caused by hemorrhoids or an anal fissure, but it is not always hemorrhoids. Persistent, recurrent, or unexplained bleeding should be evaluated.
What is colorectal bleeding?
Colorectal bleeding refers to bleeding that comes from the colon, rectum, or anus. It may appear as bright red blood, maroon stool, blood mixed with stool, or black stool depending on the source.
When should I worry about rectal bleeding?
You should seek evaluation if bleeding is recurrent, persistent, mixed with stool, dark red or black, heavy, or associated with abdominal pain, weight loss, anemia, fatigue, or a change in bowel habits.
Do I need a colonoscopy for rectal bleeding?
Not always. Some causes can be diagnosed with an office exam and anoscopy. Colonoscopy may be recommended if bleeding is unexplained, persistent, mixed with stool, associated with warning signs, or if you are due for colorectal cancer screening.
Can rectal bleeding be from a fissure?
Yes. Anal fissures commonly cause sharp pain during bowel movements and bright red blood on toilet paper.
Can rectal bleeding be painless?
Yes. Internal hemorrhoids, polyps, diverticular bleeding, and some cancers may cause painless bleeding. Painless bleeding should still be evaluated if it is persistent or unexplained.
Should I see a colorectal surgeon for rectal bleeding?
A colorectal surgeon can evaluate both anorectal and colorectal causes of bleeding, including hemorrhoids, fissures, polyps, inflammatory disease, and cancer-related concerns.
What Is Colorectal Bleeding?
Colorectal bleeding refers to bleeding from the colon, rectum, or anus. It may appear as bright red blood, blood mixed with stool, maroon stool, or black stool depending on the source.
While hemorrhoids and fissures are common causes of bright red bleeding, colorectal bleeding can also come from polyps, inflammatory bowel disease, diverticular disease, infection, or colorectal cancer.
Learn More About Rectal bleeding
You may also explore these guides:
Reviews & Testimonials
Contact
Please don't hesitate to call us at 602-932-5660 or reach out via our online form, YouTube, Instagram and TikTok for educational resources.
